Outbreaks Don’t Just Happen -We Fuel Them
 Photo by IKP Studios
Photo by IKP Studios
I went from studying cellular machinery, the intricacies of ribosome function for protein synthesis during my undergraduate degree to testing chemical disinfectants on a multi-drug resistant yeast in a biosafety level 2 laboratory during my professional training year in England. To build on this knowledge, I went back to school for a postgraduate degree, where I had the opportunity to learn from exceptional researchers and take courses such as Medical Anthropology and Conflict & Health. These experiences deepened my understanding of the sociological dimensions and consequences of health and illness. Then COVID-19 happened.
While studying about the exponential transmission of infectious diseases in my challenging Epidemiology lectures, our world was thrown into this century’s first pandemic, turning my in-person pursuit of knowledge to online learning as I had travelled back to Nigeria for the holidays just before the world went into lockdown. Though unanticipated, but deeply appreciated, I had the privilege of serving the leadership of Nigeria’s disease control agency during the pandemic. While diligently wearing my facemask and practicing social distancing, I became a pro at reviewing infectious disease guidelines, coordinating critical meetings with government stakeholders, and preparing meeting notes and presentations dedicatedly for high-level meetings with the National Economic Council, and Presidential Steering Committee on COVID-19.
 Photo by IKP Studios
Photo by IKP Studios
What a time! The last ten years of my life have been a beautiful, challenging, exciting, and time-consuming period of embracing science, its complexities, and finding my place in protecting population health. The germs that cause diseases like cholera, mpox, Lassa fever, HIV, tuberculosis, and malaria will leave you in awe if you study them. The diseases they cause though . . . not so much.
Unfortunately, the structure, orderly processes, and even beauty of these germs under a microscope are a distraction from the horror, pain, loss, and expense that follow infection. With the centuries of scientific research into infectious diseases, inestimable financial investments into medical studies, why have we heard reports of healthcare workers dying of Lassa fever in the past month in Nigeria (1)? How is it that the US battles with measles outbreaks (2) after upholding elimination status for this disease for so long. And why in the world is the headline about the spread of an unfamiliar infectious disease gracing our social media timelines in 2026 without advance notice. Nipah virus (3) anyone?
Let’s take cholera for example. Contracted through contaminated water or food, this awful disease can leave an infected person with rice-water stool, weakness, and severe dehydration (4). Nearly 200 years after John Snow traced its transmission (5), cholera remains a serious public health threat. Thought to have caused the death of the twelfth U.S. president (6) in 1850, it still claims lives in parts of Africa, the Eastern Mediterranean, and South-East Asia. In many places, conflict fuels its spread by destroying water systems, disrupting health services, and forcing people from their homes.
In regions enjoying the sanctity of life without conflict, outbreaks like cholera can be pinned to governance failures. ‘Open defecation. Lack of potable drinking water in some rural areas and urban slums; water shortage leading to reliance on people selling water in jerry cans. Inadequate health facility infrastructure and cholera commodities for management of patients (Ringer’s lactate and ORS) (7) . These are some of the challenges that strike me as issues that should have been solved centuries ago. Why is there still a need to advocate to governments to make them see the importance of providing water and sanitation infrastructure for their people? It is mind-boggling.
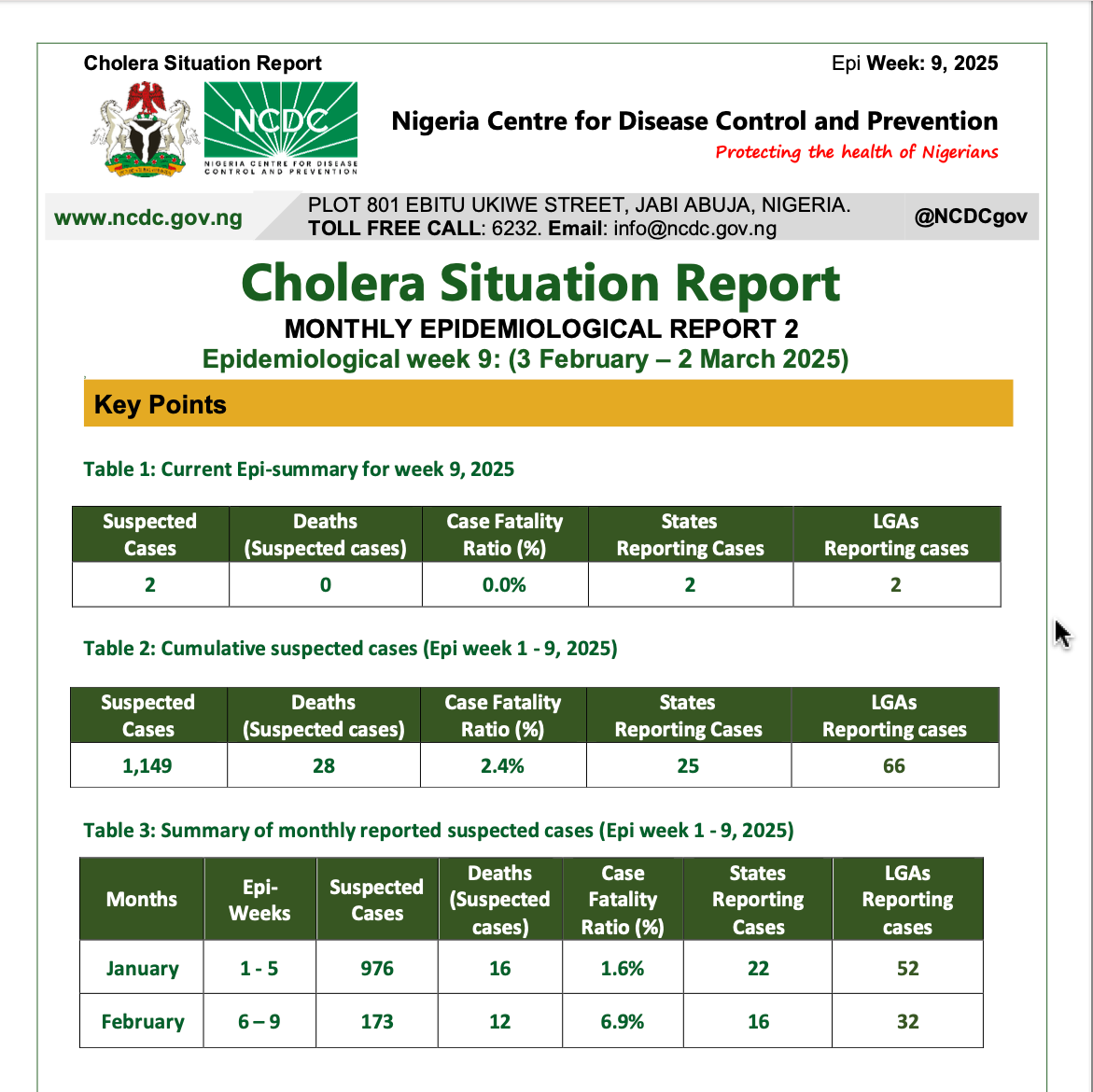 Cholera Situation Report, 2025, NCDC
Cholera Situation Report, 2025, NCDC
Working with the Nigeria Centre for Disease Control and Prevention (NCDC), I truly came to appreciate how important the agency is, not just to our health and wellbeing, but to our lives and livelihoods. One institution can be that critical to Nigeria’s Gross Domestic Product. I am deeply convinced that if there had been no government agency for infectious disease control in 2020, our response to COVID-19 would have been entirely different, and certainly not for the better.
When states report outbreaks to the NCDC, after completing their internal notifications, this triggers rapid risk assessments and, where necessary, the activation of the national Emergency Operations Centre (EOC) to coordinate disease detection, response, and control. Under the EOC, pillars such as infection prevention and control, risk communication, laboratory services, surveillance, and case management -among others- work within clearly defined roles to support affected states. That support may include deploying rapid response teams, providing logistics, dispatching critical commodities, and receiving samples for central laboratory testing.
There is a lot that outbreaks entail. But what working with the NCDC showed me is that it is possible to move from the idea of managing diseases to the reality of doing so – through intentional and strategic planning, willing, energetic, and competent Human Resources, partner support, government stakeholder buy-in, and leadership with heart.
While outbreaks occur for many of the reasons detailed in the early 2025 Cholera Situation Report – alongside broader challenges of national governance – there is also the issue of self-governance. Hygiene still seems like a myth to some educated people, while some who lack formal education may simply not know the importance of thoroughly washing their hands between using the toilet and preparing a meal.
Certainly, we need to reach those who do not know, but for those who are quick to mention their university degrees within minutes of meeting someone new, those degrees should show in how they manage illness and help prevent it. Why are you still sneezing into your hands and then shaking someone’s hand in 2026? How are you leaving the toilet without washing your hands properly with soap and water?
Outbreaks are not just biological events; they are also social, behavioural, and, most importantly, failures of governance. Water and sanitation infrastructure can be weak or non-existent, and everyday habits can cause germs to spread. But we must remember: outbreaks don’t just happen, we fuel them through our actions and inactions.